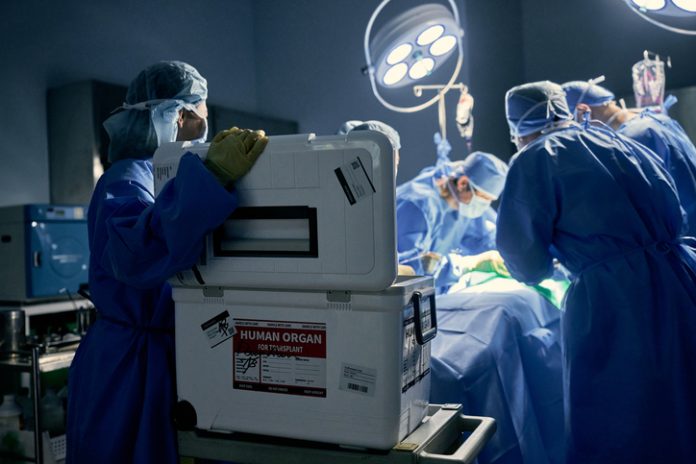
A medical protocol that expands the pool of live donor organs is getting increased attention from doctors and patient advocates who say it skirts the legal definitions of death.
The practice, known as normothermic regional perfusion with controlled donation after circulatory death (NRP-cDCD), involves inducing brain death in terminal patients by clamping their carotid arteries and restarting their hearts to keep the organs viable. Three hospitals—in Arizona, Nebraska, and New York—are conducting clinical trials to expand the practice, Medpage reported in September.
Patient advocacy groups, such as Respect for Human Life, are warning the public about the ethical problems of NRP-cDCD. Heidi Klessig, M.D., wrote, “Don’t become a victim of unethical organ harvesting practices. Don’t sign that donor card!” in American Thinker.
Potential Conflicts
Patients receiving critical care in hospitals and other medical facilities may not understand the processes by which clinical death is determined or organs may be harvested.
A 2006 revision of the Uniform Anatomical Gift Act allows hospital administrators to take organs from incapacitated patients determined to have irreversible brain function and whose family members are not reachable, Klessig told the Heartland Daily Podcast, on November 28.
“[This] is terrifying when there is a person whose interest is how much money can be made from your organs, not what is in your best interests,” said Klessig.
Live organ transplants can reap millions of dollars for hospitals that procure the organs and the centers that transplant them. According to a report by the consulting firm Milliman, the average billed charges for a heart transplant in 2020 amounted to $1,664,800. Lung transplants were billed at an average of $1,295,900 and intestines at $1,240,700.
No Shelf Life
Unlike tissue from cadavers, vital organs such as the heart, lungs, livers, and kidneys cannot be harvested from a patient whose circulatory system has shut down, says Klessig.
“These organs rely on a continuous supply of oxygen and nutrition through the bloodstream to remain viable,” said Klessig. “They are so complex that once the blood flow stops, they very quickly break down and become unsuitable for transplant.”
This explains why around 100,000 patients remain on an organ waiting list despite 1.5 million people registered organ donors dying each year, says Klessig.
“If a dead person could donate organs, that would work out to 15 organs per waiting recipient which is a lot more than we need,” said Klessig. “So clearly, dead people cannot donate organs and we wouldn’t have a waiting list at all but an organ surplus.”
An exception to the rule is a kidney or a lobe of the liver, which can be donated by patients who remain alive.
Defining Death Down
The current clinical definition of death arises from the 1968 “Report of the Ad Hoc Committee of the Harvard Medical School to Examine the Definition of Brain Death,” which replaced previous standards for determining death based on the failure of the circulatory, respiratory, and neurological systems.
The Harvard report led to the federal Uniform Determination of Death Act (UDDA), which redefined death as either (1) irreversible cessation of circulatory and respiratory functions, or (2) irreversible cessation of all functions of the entire brain, including the brain stem.
Allowing for a clinical diagnosis of “brain death” opened the door to certifying the death of a patient whose heart and lungs were still providing oxygenated blood to organs, and thereby created a convenient new avenue to live organ harvesting. The UDDA requires determinations of brain death to be rendered according to “accepted medical standards,” but there is no existing medical requirement beyond clinical observation.
“Irreversible cessation of heart and lung function OR irreversible function of the entire brain, including the stem doesn’t sound terribly controversial but the devil is in the details,” said Klessig. “The problem is that doctors are not always able to determine what is irreversible.”
‘Better Solutions for People’
In 2021, the American College of Physicians stated the NRP-cDCD procedure raised “profound ethical questions regarding the determination of death, respect for patients, and the ethical obligation to do what is best.”
Medical practice should not condone taking the life of one person to save another, says Klessig.
“I really believe if we hadn’t been pouring all our time, money, and research dollars into the current unethical system, I think we would have found better solutions for people, such as augmenting the heart or providing an artificial one,” said Klessig. “Those treatments need to be developed and those scientific pursuits are not being funded.”
Organ procurement is big business with less and less concern for donors’ welfare and lives, says Julie Grimstad, a board member and patient advocate at the Healthcare Advocacy and Leadership Organization (HALO).
“There have been efforts to develop animal transplants; none of them have been successful,” said Grimstad. “There have also been efforts to develop mechanical organs, such as a permanently implanted pump that would act as an artificial heart. A wonderful physician, Harold Kletschka, M.D., developed a successful working model decades ago, but it never went to market due to several unsavory efforts to take control of the project.”
A biography on Kletschka, To Change the Heart of a Man, was published in 2009.
Kevin Stone (kevin.s.stone@gmail.com) writes from Arlington, Texas and
AnneMarie Schieber (amschieber@heartland.org) is the managing editor of Health Care News.
Internet info:
“Think Twice Before Signing that Organ Donation Card – Heidi Klessig, M.D.,” The Heartland Daily Podcast, November 28, 2023.