A congressional hearing examined the value of tax breaks and subsidies for non-profit hospitals compared to the charitable services they provide.
The Subcommittee on Oversight of the House Ways and Means Committee received testimony on whether non-profits provide charity care and community benefits commensurate with the tax benefits they get, at an April 26 hearing.
Subcommittee Chairman David Schweikert (R-AZ) said non-profit hospitals are required to provide services for the subsidies they receive.
“Hospitals must meet certain standards to obtain and maintain tax-exempt status, including organizational and operational requirements, community benefits, and Patient Protection and Affordable Care Act (ACA) requirements,” said Schweikert.
The value of the tax exemptions for nonprofit hospitals rose from about $19 billion in 2011 to around $28 billion in 2020, with half of that amount coming from the federal tax exemption, according to the Kaiser Family Foundation (KFF).
Lax Oversight
There are disparities in the amount of free or discounted health care individual hospitals provide, unrelated to their size or revenues, said Schweikert.
“KFF has also found that the value of charity care provided by hospitals varies substantially across facilities, ranging from 0.1 percent of operating expenses for a hospital to 7 percent or more for other hospitals,” said Schweikert.
This range is likely the result of the failure to spell out the service obligations of nonprofit hospitals in federal law and regulations, said Schweikert.
“The wide variation here appears to come from the lack of clear guidance from Congress and the IRS about what constitutes community benefit,” said Schweikert.
Net Worth Rising
Auditors at the transparency group OpenTheBooks.com found the cumulative net assets of the 20 non-profit hospital systems grew from $200.6 billion in 2018 to $324.4 billion in 2021.
The non-profit hospitals received $23 billion in COVID pandemic bailouts, but only two providers have paid the money back, OpentheBooks CEO Adam Andrezejewski told Health Care News.
“For every $1 in COVID bailout money, the net assets of the top 20 largest non-profits jumped $5,” said Andrezejewski. “Non-profit hospitals need to explain if they are serving the public’s interests or their own.”
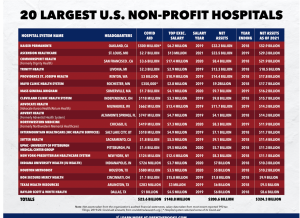
(graphic courtesy OpenTheBooks)
CEO Compensation
The salaries of CEOs at non-profit hospitals are a concern, Ways and Means Committee Chairman Jason Smith (R-MO) said at the hearing.
“The level of executive compensation is particularly alarming,” said Smith. “The top 10 non-profit hospital CEOs average more than $7 million annually. Some as high as $14 million. This further questions whether these facilities are living up to their mission statements.”
OpenTheBooks estimates that the top executives at the 20 largest non-profit hospitals in the United States receive a total of $148.8 million in annual compensation, based on these hospitals’ latest publicly available tax filings. For example, the CEO at Ascension Healthcare, based in St. Louis, Missouri, made $13 million in 2021.
How Nonprofits Profit
The discounted drug prices non-profit hospitals receive from drug makers through the federal 340B Drug Pricing Program are also a concern, said Smith.
The mandatory discounts are meant to reimburse providers that serve low-income patients, including hospitals serving Medicaid and uninsured patients.
But hospitals profit from the 340B program by getting drugs at discounted prices and then charging insurance companies and Medicare the full price, Ge Bai, Ph.D., a professor of accounting at Johns Hopkins Carey Business School, and a witness at the hearing, told Health Care News.
“This ‘buy-low-sell-low’ 340B program for safety-net hospitals has evolved into a ‘buy-low-sell-high’ program for eligible tax-exempt hospitals, who can generate substantial profits by providing these drugs to well-insured patients,” Bai said.
“To take advantage of the 340B program, many tax-exempt hospitals have acquired or affiliated with clinics located in wealthy communities and then shifted care away from outpatient physician offices to more expensive hospital outpatient centers,” said Bai.
Bonner Russell Cohen, Ph.D. (bcohen@nationalcenter.org) is a senior fellow at the National Center for Public Policy Research.





















